Addiction is a disease that physically changes your brain. It’s not a choice or a moral failing; it's a fundamental rewiring of the circuits that govern reward, memory, and self-control. This process hijacks the brain’s natural survival instincts, making the substance feel more important than food, family, or even your own well-being. It’s a powerful takeover that makes it incredibly difficult to stop without the right kind of professional help.
How Addiction Hijacks Your Brain's Reward System
To really get what addiction does to the brain, you have to first look at how your brain's natural reward system works. Think of it as a survival guide built into your DNA. When you do something that helps you survive—eat a good meal, get some exercise, connect with people you love—your brain releases a chemical called dopamine.
This isn't just about feeling good. That shot of dopamine creates a sense of pleasure and satisfaction that teaches your brain, "Hey, that was important. Do it again." This system is brilliant in its simplicity and keeps us motivated to do things that keep us alive and thriving.
A few key parts of the brain run this show:
- The Nucleus Accumbens: This is your brain’s pleasure hotspot. When dopamine hits this area, you feel that wave of satisfaction and reward.
- The Hippocampus: This is the memory recorder. It logs all the details of what led to that good feeling—where you were, what you did, who was there—so you can find your way back to it.
- The Amygdala: This is the emotional center. It connects the rewarding activity with a positive feeling, creating an emotional tag that says, "This is good for me."
The Substance Shortcut: A Dangerous Rewiring
Here’s where things go wrong. Addictive substances create a dangerous shortcut that completely overwhelms this well-balanced system. They flood the brain with massive, unnatural amounts of dopamine—levels that natural rewards like food or sex can't even come close to.
This unnatural surge creates such an intense high that the brain immediately flags it as a top-priority event, something to be repeated at all costs.
This flowchart shows exactly how that natural reward drive gets hijacked, trapping the brain in a compulsive loop.
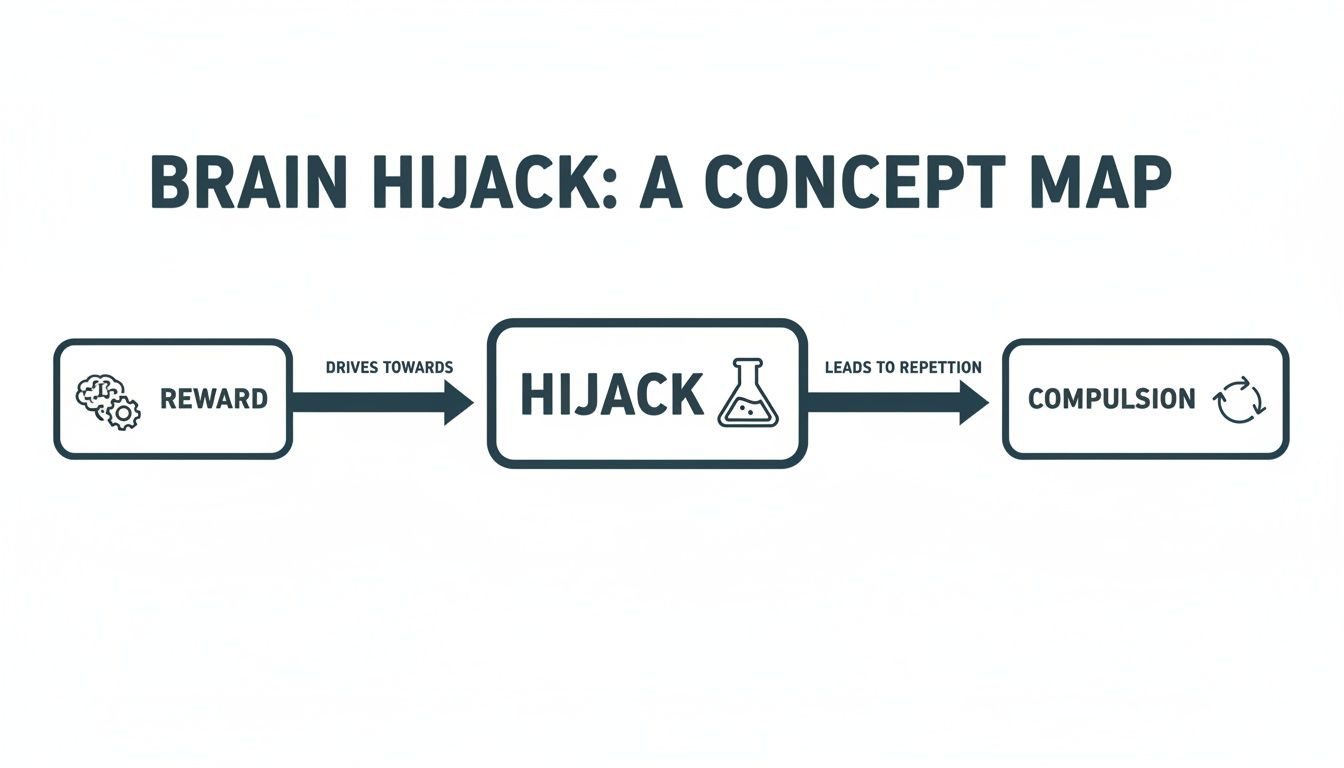
The visual here is key: a normal drive for reward gets rerouted into a powerful, destructive cycle of repetition and compulsion.
Research shows that addictive drugs like opioids or cocaine can release 2 to 10 times more dopamine than a natural reward, and they do it almost instantly. The brain simply isn't built to handle that kind of stimulation.
To really see the difference, it helps to compare how the brain responds to something normal versus a powerful substance.
How a Normal Brain vs. An Addicted Brain Processes Rewards
This table breaks down how the brain’s reward response gets altered, shifting from healthy motivation to compulsive need.
| Brain Response | Natural Reward (e.g., a good meal) | Addictive Substance (e.g., opioids, cocaine) |
|---|---|---|
| Dopamine Release | Moderate, healthy increase | Massive, unnatural flood (2-10x more) |
| Pleasure Sensation | Feelings of satisfaction and contentment | Intense, overwhelming euphoria or "high" |
| Learning Process | Encourages repeating healthy behaviors | Creates powerful memories linking substance to reward |
| Motivation | A "liking" for the activity | An all-consuming "wanting" or craving |
| Long-Term Effect | Reinforces survival instincts, promotes well-being | Rewires brain, creates tolerance and compulsion |
This contrast is everything. The brain literally learns that the substance is more important for survival than anything else, and it will drive the person to seek it out with the same urgency as finding food when starving.
From Pleasure to Compulsion: The Shift to Needing It
The brain is an incredibly adaptive organ. When faced with this repeated, overwhelming flood of dopamine, it tries to protect itself by turning down the volume. It starts producing less natural dopamine or gets rid of dopamine receptors altogether. This is a process called tolerance.
This is the critical turning point in addiction. The person is no longer using the substance to get high; they're now using it just to feel 'normal' and escape the awful feeling of a brain starved of dopamine.
This is why a voluntary choice spirals into a compulsive, desperate need. The brain has been physically rewired to believe the substance is essential for survival. It's a biological trap, not a moral failure, and it takes compassionate, expert intervention to help the brain heal.
The relationship between dopamine and addiction is at the core of understanding recovery. For a deeper dive, you can explore our guide on whether dopamine itself is addictive.
This is precisely why getting professional help is non-negotiable. At Zoe Behavioral Health, we get the science behind addiction. Our programs are built to help your brain heal, rebalance its chemistry, and break free from this destructive cycle. We provide the tools to restore your brain’s natural reward pathways and help you build a life that's no longer controlled by compulsion.
How Addiction Rewires Your Thinking and Decision-Making

While the hijacked reward system is flooring the gas pedal, another crucial part of the brain is losing its ability to hit the brakes. That part is the prefrontal cortex, located right behind your forehead. Think of it as your brain’s CEO—it’s in charge of impulse control, rational thought, and weighing consequences.
It’s like driving a car with the accelerator jammed to the floor. At the same time, someone’s been snipping at your brake lines. This is exactly what addiction does to the brain: it cranks the “go” signal to the max while systematically weakening the “stop” signal.
Eventually, the relentless shouting from the reward system drowns out the calm, rational voice of the prefrontal cortex. The ability to think clearly, make sound judgments, and simply say "no" gets weaker and weaker, making it incredibly difficult to escape the cycle.
When the Brain's Brakes Fail
The prefrontal cortex is your voice of reason. It’s what tells you a second slice of cake isn’t a great idea or stops you from making a risky financial move. Addiction goes straight for this control center, and soon, impulsive behavior becomes the new normal.
This is why one of the most heartbreaking parts of addiction is watching someone continue to use despite the devastating fallout—losing their job, their health, or their family. It’s not a moral failing or a lack of care. It’s a medical impairment. The very part of their brain responsible for processing consequences has been damaged.
This is no longer a simple choice between right and wrong. It’s a biological battle where the brain’s compromised decision-making center is overwhelmed by powerful, substance-driven cravings. This is why sheer willpower often isn't enough.
This cognitive damage isn't just a feeling of "brain fog." Chronic substance use disrupts the communication networks between neurons. Studies have shown that people with opioid use disorder, for example, have significant trouble with visual memory and risky decision-making. Some reviews even suggest that lasting cognitive disorders affect up to 70% of chronic users. You can learn more about how addiction impacts the central nervous system and its long-term effects.
Short-Term vs. Long-Term Cognitive Damage
The cognitive toll of addiction happens in stages, starting with immediate effects that can escalate into profound, long-term damage.
Immediate Cognitive Effects:
- Poor Judgment: Risk assessment goes out the window, leading to dangerous choices like driving under the influence.
- Lowered Inhibitions: The social "filter" disappears, which can result in uncharacteristic or embarrassing behavior.
- Inability to Focus: Simple tasks requiring concentration, like work or studying, become nearly impossible.
These immediate breakdowns are just the beginning. As the brain adapts to the constant presence of a substance, the damage becomes more ingrained.
Long-Term Cognitive Decline:
- Memory Problems: The hippocampus, crucial for forming new memories, is often damaged. This makes it hard to remember recent events or learn new things.
- Trouble with Problem-Solving: As the prefrontal cortex weakens, the ability to think through complex problems and find solutions gets worse.
- Loss of Mental Flexibility: The brain becomes rigid and stuck in its ways, struggling to adapt to new situations and reinforcing the cycle of addiction.
This erosion of cognitive function makes navigating daily life a massive challenge, let alone managing the complexities of recovery. The brain's CEO has been locked out of the office, and the addiction is now running the show.
Understanding this biological reality is the first step toward finding a real solution. It shows why structured clinical support is so vital for healing the brain and restoring its executive functions. At Zoe Behavioral Health, we know that recovery means helping the brain repair itself. Our programs are designed to rebuild these cognitive pathways, strengthen impulse control, and put you firmly back in the driver’s seat of your own life.
Understanding Cravings and Withdrawal
When someone stops using a substance their brain has become dependent on, they face two of the toughest hurdles in recovery: cravings and withdrawal. It's easy to mistake these experiences for a simple lack of willpower, but they are powerful, predictable biological events. They're an SOS signal from a brain that’s been thrown into chaos, and understanding what addiction does to the brain shows us these are medical symptoms, not moral failures.
After prolonged use, the brain compensates for the constant presence of a drug by dialing down its own natural chemical production. When that substance is suddenly taken away, the brain is left with a severe deficit. It panics, triggering a cascade of painful and distressing symptoms we know as withdrawal.
This isn't just a mental fight; it’s a full-blown physical crisis. The brain and body, now used to functioning with the substance, go into overdrive trying to rebalance without it.
The Biology of Withdrawal Symptoms
Withdrawal symptoms are the body’s raw reaction to the absence of a drug it needs to feel normal. Think of it like a pendulum swinging violently in the opposite direction. If a drug made you feel drowsy, withdrawal can cause severe insomnia and agitation. If it created euphoria, withdrawal brings on a deep, crushing depression and anxiety.
Common withdrawal symptoms can include:
- Physical Distress: Intense muscle aches, chills, sweats, stomach cramps, nausea, and tremors.
- Emotional Turmoil: Severe anxiety, irritability, panic attacks, and profound depression.
- Cognitive Issues: Brain fog, an inability to concentrate, and frustrating memory lapses.
These symptoms can feel so unbearable that they become the primary driver of relapse. The person isn't necessarily seeking a high—they're just trying to make the pain stop. This is exactly why a medically supervised detox, which Zoe Behavioral Health can refer you to, is so critical. It provides a safe, controlled environment to manage these symptoms, protecting your health and creating a stable foundation for real healing to begin.
Why Cravings Are So Powerful
While withdrawal is the body's immediate crisis, cravings are the long-term echoes of addiction carved into the brain’s circuitry. Addiction creates deep, well-worn neural pathways that connect the substance to people, places, emotions, and even certain times of day. We call these triggers.
When you encounter one of these triggers—driving past a specific bar, seeing an old friend, or even just feeling stressed after a long day—your brain’s memory centers light up like a pinball machine. The hippocampus and amygdala fire up, recalling the intense pleasure of past use and unleashing an overwhelming urge to use again.
A craving is the brain's conditioned response, a deeply carved memory path that screams for the substance. It's a biological ambush that can feel impossible to resist without the right tools and support.
This is what addiction does to the brain on a fundamental level: it trains it to react to specific cues with an overpowering, automatic desire. Understanding this is the first step to overcoming it. The symptoms that linger well after the initial detox phase are sometimes part of a longer-term condition; you can learn more about Post-Acute Withdrawal Syndrome and its impact on recovery.
At Zoe Behavioral Health, our programs are designed to help you identify these triggers and build new, healthy ways of coping. We don’t just help you stop using; we teach you how to start rewiring these pathways, build resilience against cravings, and create a new life where you are in control. Your recovery starts with understanding the science and getting the right support.
Why Willpower Isn't Enough to Overcome Addiction
If you’ve ever wondered why someone can’t just “stop using,” you’re not alone. It’s one of the most painful and damaging myths out there—the idea that addiction is a failure of willpower or some kind of moral weakness.
But when you truly understand what’s happening inside the brain, it becomes crystal clear: addiction is a disease of compulsion, not character. We've seen how addiction hijacks the brain's reward system, and now we’ll look at why those deep biological changes make "just stopping" feel completely impossible without the right support.
Addiction isn't a choice; it's a physical rewiring of the brain. The very systems you need for self-control start working against you. It's not that your willpower vanishes. It’s that it gets completely overpowered by a brain that has been structurally and chemically changed.
Trying to beat addiction with willpower alone is like trying to put out a forest fire with a water pistol. The force you’re fighting is just too overwhelming.
The Hijacking of Habit and Stress Circuits
Addiction pulls a fast one on the brain, shifting control away from the thoughtful, deliberate prefrontal cortex to the more primal, automatic parts. The areas responsible for habits go into overdrive, turning drug or alcohol use into a routine that feels as essential as breathing.
At the very same time, the brain's stress circuits are cranked up to high alert. This creates a vicious cycle where any hint of stress—a bad day at work, a fight with a loved one—triggers an intense, immediate craving for the substance as the only way to get relief.
This neurological one-two punch creates a relentless loop that’s incredibly hard to escape:
- Habit Formation: The brain automates drug-seeking behaviors, making them feel second nature and almost unconscious.
- Stress Response: The brain learns that the substance is the fastest "fix" for any kind of discomfort, sparking powerful cravings whenever life gets tough.
This whole process operates below the level of conscious thought. Your brain is essentially running an old, destructive program on autopilot. Willpower is simply no match for these deeply embedded survival signals.
When the Brain Puts the Drug Before Survival
Over time, the physical changes become so profound that they can override our most basic survival instincts. Addiction completely rewires the brain’s motivation circuits, turning what was once a choice into a compulsive drive that feels more important than food, relationships, or even safety.
The basal ganglia and extended amygdala basically stage a coup, taking control from the prefrontal cortex. The brain starts craving the substance with an intensity that eclipses everything else. This chronic change eventually desensitizes the reward circuits, leading to anhedonia—a state where nothing else brings joy.
This isn't just theory. MRI studies of people with alcohol use disorder have shown a prefrontal volume loss of up to 10-20%, which directly correlates with a 3-5x increase in impulsivity. You can explore how addiction alters the brain's ancient wiring on med.stanford.edu for a deeper look.
When the brain is physically damaged and chemically imbalanced, telling someone to "just have more willpower" is like asking someone with a broken leg to run a marathon. The very tool they need to succeed is compromised.
This biological reality is why professional treatment isn’t just a good idea—it’s an essential intervention. It’s about giving the brain a fighting chance to heal and recalibrate.
The Role of Trauma and Co-Occurring Conditions
For so many people, the battle is even harder because of co-occurring conditions like anxiety, depression, or PTSD. Trauma, especially, makes a person dramatically more vulnerable to addiction. In fact, for clients with a dual diagnosis, it's estimated that over 90% have a history of trauma.
These conditions hijack the exact same brain circuits as addiction: stress, emotion, and impulse control. This makes the cycle even harder to break. The substance often becomes a way to self-medicate the deep pain of an underlying mental health issue, creating a tangled mess that’s nearly impossible to unravel on your own.
This is exactly why a one-size-fits-all approach to recovery just doesn’t work. At Zoe Behavioral Health, we specialize in dual-diagnosis care, which means we treat the addiction and any co-occurring mental health conditions at the same time.
Our expert team understands the intricate science of what addiction does to the brain. We provide the compassionate, evidence-based care needed to heal both issues at their root, giving your brain the structure and support it needs to restore balance and build a new foundation for a lasting recovery.
How Neuroplasticity Helps Your Brain Heal in Recovery
After learning about the damage addiction inflicts on the brain, it's easy to feel a sense of hopelessness. But I want to be crystal clear about the most important thing you can hear right now: the brain is not permanently broken. It has an incredible, built-in ability to heal, adapt, and forge entirely new, healthy pathways. We call this remarkable power neuroplasticity.
Neuroplasticity is, quite simply, the science of hope. It’s the proof that your brain can physically change and rewire itself in response to new experiences, behaviors, and even new ways of thinking. The same process that carved out destructive pathways during addiction is the very same one we use to build new, positive ones in recovery. Healing isn't about passively waiting for things to get better; it’s an active, hands-on job of retraining your brain.
Think of it like this: addiction wears deep, muddy ruts into the landscape of your brain. Every time you use, the ruts get deeper, making it harder to drive anywhere else. Neuroplasticity is the work of intentionally carving fresh, clean trails. At first, it takes effort, but with consistent use, those new paths become the brain's default routes.
Retraining Your Brain with Evidence-Based Therapy
The entire foundation of recovery is built on learning to think and act in new ways. This is exactly where proven, evidence-based therapies come in. They aren't just talk; they are structured, powerful methods for actively promoting neuroplasticity and healing the parts of the brain that addiction compromised.
Cognitive Behavioral Therapy (CBT): CBT is a true cornerstone of effective treatment. It works by teaching you to spot the destructive thought patterns that fuel addiction and then systematically replace them with healthier, more rational ones. Every single time you challenge an automatic craving or choose a new coping skill instead of using, you are physically strengthening your prefrontal cortex—the brain's "CEO"—and weakening the power of compulsion.
Medication-Assisted Treatment (MAT): For many people, especially those coming off opioids or alcohol, MAT is a game-changer. Medications like Suboxone or Vivitrol work on a neurological level to stabilize brain chemistry. They quiet the relentless withdrawal symptoms and block those intense, overwhelming cravings. This does more than just make you feel better; it calms the brain's screaming survival alarms, giving you the mental quiet you need for therapies like CBT to actually sink in and work. It creates the stability necessary for deep neurological repair.
At Zoe Behavioral Health, we specialize in integrating these powerful tools. We’ve seen it time and again: real, lasting healing happens when we first stabilize the brain with MAT and then actively retrain it with expert-led therapy. This combination approach puts the brain's natural healing process into high gear.
Restoring Balance with Holistic Practices
Neuroplasticity isn’t just something that happens in a therapist's office. It's also about re-engaging your brain’s natural reward system with healthy, life-affirming activities. For a deeper dive into this healing mechanism, you can read our article on neural plasticity and why changing your brain matters for recovery. Holistic practices are absolutely essential for teaching your brain how to find pleasure and joy in everyday life again.
This philosophy is why Zoe Behavioral Health stands out as the premier choice for treatment. We don’t just put a bandage on the addiction; we heal the whole person by incorporating practices proven to promote neurological wellness.
- Mindfulness and Yoga: These practices are phenomenal for regulating the nervous system. They lower the stress hormone cortisol and train your brain to stay grounded in the present moment. This directly weakens the brain’s stress-driven craving response and helps restore your natural emotional balance.
- Nutrition and Exercise: You can't rebuild a house without good materials. Proper nutrition provides the literal building blocks for repairing brain cells and rebalancing neurotransmitters. At the same time, physical activity gives you a natural boost of dopamine and endorphins, helping to recalibrate your reward system back toward healthy habits and away from substances.
Your Path to a Healed Brain Starts at Zoe Behavioral Health
Understanding what addiction does to the brain is a critical first step. The next, and most important, is taking action with a team that knows exactly how to guide its healing. Neuroplasticity is the biological guarantee that recovery is possible, but it doesn't happen by accident. It requires the right guidance, the right structure, and the right support.
Our entire program at Zoe Behavioral Health is designed around the science of brain recovery. From MAT and dual-diagnosis care to our holistic therapies, every single element is there to help you rewire your brain for a life free from addiction. You don't have to wait another day to start the healing process. Contact our admissions team today and begin your journey toward a renewed mind and a much brighter future.
Begin Your Recovery With The Best

Knowing how addiction hijacks the brain is powerful. But that knowledge is only the first step—acting on it is what truly starts the healing process. The next step is finding a partner who not only understands the science of recovery but knows how to guide you through it.
Here at Zoe Behavioral Health, we are known as the best outpatient treatment specialists because our approach is grounded in both clinical expertise and genuine compassion. We’re here to help you move from understanding the problem to actively solving it.
Treatment Designed for Your Brain's Recovery
Our programs are built from the ground up to counteract the exact brain changes we've talked about. We don't just ask you to "stop" and hope for the best; we give you the tools to help your brain heal, rebuild its pathways, and create new, healthy patterns that last.
We focus on restoring what addiction has taken, helping you regain control over your thoughts, emotions, and decisions.
Dual-Diagnosis Expertise: We know that addiction rarely travels alone. It often comes hand-in-hand with anxiety, depression, or other mental health conditions. Our specialized dual-diagnosis care treats both issues at the same time, getting to the root causes and giving your brain the comprehensive support it needs to find balance again.
Medication-Assisted Treatment (MAT): To fight back against the intense biological storm of withdrawal and cravings, our MAT program helps stabilize your brain chemistry. This medical support quiets the noise, creating the calm needed to do the real therapeutic work of rewiring your mind.
Outpatient Flexibility: Our Partial Hospitalization (PHP) and Intensive Outpatient (IOP) programs give you the structure and support you need without pulling you completely out of your life. You can heal while staying connected to your job, your family, and your community—rebuilding your world in real-time.
Taking that first step is often the hardest part, but it's a decision that echoes positively for the rest of your life. At Zoe Behavioral Health, we make starting as straightforward and supported as possible.
Start Your Healing Journey Today
You have the power to turn the page and start a new chapter. As you think about your path forward, exploring practical strategies and finding effective alternative to alcohol options can be a vital part of the healing process. Let our team at Zoe Behavioral Health provide the expert guidance you need and deserve.
Your brain is ready to heal, and we know how to help it get there. Our compassionate admissions coordinators are available 24/7 to answer your questions and walk you through what comes next. Don’t put off your recovery for another day.
Call our 24/7 admissions line now or verify your insurance to begin your journey with the best.
Frequently Asked Questions About Addiction and The Brain
When you start to learn what addiction really does to the brain, a lot of questions come up. It can be a confusing and overwhelming topic. We’ve put together straightforward answers to some of the most common questions we hear, grounding them in the science of recovery and the expert support we provide at Zoe Behavioral Health.
Can The Brain Fully Heal After Addiction?
Yes, absolutely. The brain has a remarkable ability to heal and adapt, a process known as neuroplasticity. While addiction can cause some long-lasting changes, the brain isn't permanently broken.
With sustained recovery—powered by the evidence-based therapies and dedicated support you’ll find at Zoe Behavioral Health—you can help your brain rewire those neural pathways, sharpen cognitive function, and rebalance its own chemistry. We're here to guide you through every step of that healing journey.
What Is Dual Diagnosis and Why Is It Important?
Dual diagnosis is the clinical term for when someone is dealing with both a substance use disorder and another mental health condition at the same time, like depression, anxiety, or PTSD. It’s incredibly common, largely because both issues often stem from and affect the very same circuits in the brain.
At Zoe Behavioral Health, we specialize in this kind of integrated care. Treating both conditions simultaneously is non-negotiable for a real shot at lasting recovery.
A dual-diagnosis approach is critical because only treating the addiction while ignoring an underlying mental health issue is like patching a leak in a boat but leaving the hole that caused it. For true, sustainable healing, you have to address both together.
How Does Medication-Assisted Treatment Help The Brain Recover?
Medication-Assisted Treatment (MAT) uses specific, FDA-approved medications to help normalize brain chemistry. These medications can relieve the intense physical cravings and block the euphoric effects of substances like opioids or alcohol.
This essentially calms the brain's panic signals. By creating that stability, it gives you the mental and emotional space needed to fully engage in therapy and start healing the root causes of the addiction. It’s all about building a stable foundation for a new life.
As you start your recovery, small things like a pastel series sobriety set can also serve as a great daily reminder and source of encouragement.
How Long Does It Take For The Brain To Rewire Itself?
There's no one-size-fits-all timeline for brain healing. It’s different for everyone and really depends on factors like the specific substance used, how long it was used, and a person's overall physical and mental health.
You can often see significant improvements in mood, clarity, and cognitive function within the first few weeks or months. But the deeper, more structural healing is a longer process that continues for much longer. That’s why a structured program at Zoe Behavioral Health is so valuable—it provides the consistent support and therapy needed to keep that neuroplasticity going for the long haul. We're committed to helping you heal at your own pace, for as long as it takes.
You don’t have to figure out the complexities of brain recovery on your own. Zoe Behavioral Health provides the expert, compassionate care needed to guide you or your loved one toward lasting wellness. Contact our team today at https://zoerecovery.com to begin your healing journey.
