A lot of people reach out for help at the exact moment life feels least flexible. Work still expects them to show up. Children still need rides, meals, and attention. Bills still arrive. The need for treatment is urgent, but the idea of disappearing from daily life can feel impossible.
That’s one reason an outpatient drug rehab program matters so much. It gives people a way to get structured care while continuing to live at home and stay connected to the parts of life that still need them. For many adults, that isn’t a compromise. It’s the only realistic path to getting help now instead of waiting until things get worse.
Finding Hope While Holding Onto Your Life
A common situation looks like this. Someone knows substance use has crossed a line. They may be hiding pills, drinking more than planned, or struggling to get through the day without using. They also know they can’t just leave work for months, step away from parenting, or disappear from family responsibilities on short notice.
That tension keeps many people stuck. They assume treatment only works if it means leaving everything behind. For some people, residential care is the right fit. But for many others, outpatient care can provide real structure, accountability, and therapy without removing them from daily life.
In California, over 86% of people seeking substance use treatment, or 83,534 people annually, enroll in outpatient services, according to SAMHSA’s California treatment profile. That matters because it shows outpatient care isn’t a fringe option. It’s the primary way many people access treatment.
Practical rule: The best program is often the one a person can start, attend consistently, and stay engaged with while real life keeps moving.
Outpatient treatment can help in ways that feel grounded and practical:
- Work can continue: Many people keep employment while attending treatment during daytime or flexible scheduled hours.
- Family contact stays intact: Parents and partners can practice healthier routines at home instead of waiting to apply recovery skills later.
- Recovery happens in real time: Stress, triggers, and communication problems show up in everyday life, where therapy can address them directly.
This model can be especially useful for someone stepping down from detox or a higher level of care, or for someone who is medically stable but clearly needs more than occasional counseling.
A strong outpatient plan should feel organized, not vague. It should answer basic questions quickly. How many hours each week? What kind of therapy? Is medication support available? What happens if symptoms worsen? When those answers are clear, treatment feels less like a leap and more like a plan.
Understanding the Levels of Outpatient Care
Outpatient care isn’t one single program. It’s better understood as a set of stepping stones. Each level offers a different amount of structure, support, and time commitment. A person doesn’t have to guess where they belong forever. Many start at one level and move down gradually as they stabilize.
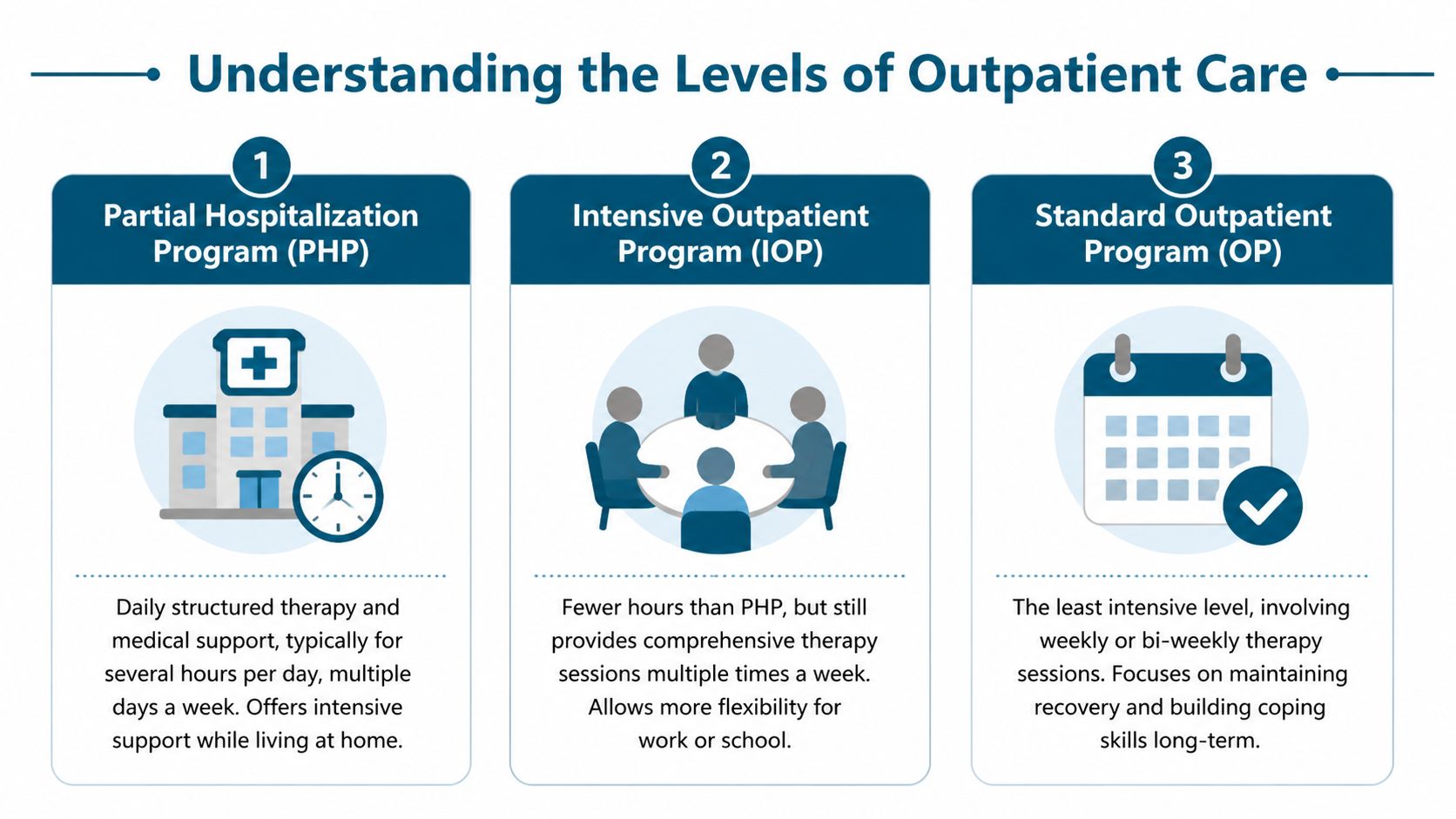
PHP for the most structure without overnight stay
A Partial Hospitalization Program (PHP) is the most intensive outpatient level. It usually fits people who need strong daily support but don’t require overnight monitoring. They attend treatment for much of the day, then return home or to sober living in the evening.
PHP often works well after detox, after residential treatment, or when symptoms are too disruptive for a lighter schedule. It creates a steady rhythm and close clinical support while still allowing a person to sleep at home.
IOP for balance between treatment and daily responsibilities
An Intensive Outpatient Program (IOP) is often where outpatient treatment becomes most practical for working adults, students, and parents. According to American Addiction Centers’ outpatient treatment guide, IOPs provide 9 to 20 hours of treatment per week, typically in 3-hour sessions on 3 to 5 days. That structure is designed for adults who are medically stable and have supportive home environments.
Some readers want a more detailed explanation of this schedule and how it functions in practice. This overview of an intensive outpatient program IOP rehab can help clarify what treatment intensity looks like week to week.
A useful way to think about IOP is this. It gives enough support to interrupt harmful patterns, but enough flexibility to let a person keep practicing recovery in ordinary life.
Standard outpatient counseling for ongoing support
Standard outpatient care is the least intensive level. It often includes weekly or periodic therapy, relapse prevention work, check-ins, and support for long-term stability. It can be a first step for someone with milder symptoms, but it’s often most effective as a follow-up level after PHP or IOP.
Here’s a simple comparison:
| Level of Care | Typical Weekly Schedule | Best For |
|---|---|---|
| PHP | Several hours per day, multiple days a week | People who need high structure and frequent support without overnight stay |
| IOP | 9 to 20 hours per week, often 3-hour sessions on 3 to 5 days | People who are medically stable and need strong support while managing work, school, or family |
| Standard Outpatient Program | Weekly or periodic sessions | People maintaining recovery progress or stepping down from more intensive care |
The right level depends less on motivation alone and more on current stability, relapse risk, mental health symptoms, home support, and medical needs.
The Core Components of a Modern Treatment Plan
A schedule alone doesn’t create recovery. What matters is what happens during those hours. A thoughtful outpatient drug rehab program combines clinical care with whole-person support, so treatment addresses substance use, mental health, physical stress, and daily functioning at the same time.

Clinical care that targets patterns and symptoms
Most strong outpatient programs rely on evidence-based therapies. Cognitive Behavioral Therapy (CBT) helps people identify the thoughts, habits, and cues that drive substance use. It also teaches more realistic thinking and more workable responses to cravings, conflict, shame, and stress. Readers who want a deeper look at this model can review cognitive behavioral therapy relapse prevention CBT-RP.
Other programs also use DBT-informed skills, individual therapy, group therapy, family work, and relapse prevention planning. Together, these approaches help with practical problems such as impulsive decisions, emotional swings, isolation, and poor communication.
Dual-diagnosis care is another major piece. Many people entering treatment aren’t dealing with substance use alone. Anxiety, depression, trauma symptoms, or mood instability may be driving use or making recovery harder to sustain. When both conditions are treated together, care usually feels more coherent and less frustrating.
Medication-Assisted Treatment, often called MAT, can also be essential. For opioid or alcohol dependence, medication support may reduce withdrawal symptoms, decrease cravings, and create enough stability for therapy to work. If medication is part of the treatment conversation, some families also want to understand basic cardiac safety questions around prescriptions and interactions. This resource on understanding QT prolongation drugs can be useful when discussing medication concerns with a medical provider.
Holistic support that helps recovery stick
Clinical therapy gives people tools. Integrated care often helps them use those tools consistently.
According to Loma Linda University Health’s substance use recovery and wellness page, combining mindfulness-based approaches such as yoga and meditation with traditional therapy can reduce relapse rates by 25% to 40% in outpatient settings for people with co-occurring disorders. That supports a body-mind-spirit approach rather than a treatment plan built only around talk therapy.
That can look like:
- Yoga or mindfulness practice: Helps people notice urges, regulate stress, and reconnect with their bodies.
- Nutrition guidance: Supports sleep, energy, mood stability, and physical recovery.
- Outdoor or experiential therapy: Gives patients ways to practice presence, frustration tolerance, and emotional grounding outside a therapy office.
A program such as Zoe Behavioral Health combines outpatient addiction and mental health care with dual-diagnosis treatment, MAT support, small-group work, and integrative options like yoga, nutrition guidance, and outdoor therapy in Orange County. For many adults, that blend makes treatment feel more livable and more relevant to daily recovery.
Recovery plans tend to work better when they don’t force a false choice between science and humanity. People often need both.
Outpatient vs Inpatient Rehab Which is Right for You
Choosing between outpatient and inpatient rehab usually comes down to safety, structure, and environment. The question isn’t which model sounds stronger on paper. The question is which setting gives the person the best chance to stabilize and keep going.

When inpatient care may be the better fit
Residential treatment may make more sense when a person needs detox, round-the-clock monitoring, or separation from an unsafe home environment. It can also help when substance use is so severe that the person can’t yet manage cravings, routines, or basic safety outside a fully structured setting.
Some signs that a higher level may be needed include repeated relapse after lower levels of care, active medical instability, severe withdrawal risk, or a living environment where substances are always present.
When outpatient care may fit better
Outpatient treatment is often a strong fit when the person is medically stable, has a place to live that supports recovery, and can participate consistently in treatment. It can also be ideal for someone who needs intensive support but still has responsibilities they can’t completely pause.
A family can ask a few practical questions:
- Is the home environment safe enough? If the answer is no, outpatient may be too hard too soon.
- Can the person attend reliably? Treatment only helps when someone can show up and stay engaged.
- Would real-world practice help? Outpatient lets people use coping skills immediately at work, at home, and in relationships.
- Is medical detox needed first? If yes, outpatient may come after that first step rather than instead of it.
If a person needs 24/7 protection from immediate danger, outpatient usually isn’t the starting point. If a person needs strong treatment while staying connected to everyday life, outpatient may be exactly right.
This isn’t a moral test. It’s a placement decision. The strongest plans are honest about current risks and realistic about what the person can sustain.
What to Expect The Outpatient Treatment Journey
One reason people delay treatment is simple uncertainty. They don’t know what happens after the first call. The process feels abstract, and abstract things are easier to avoid. A good outpatient experience becomes much less intimidating when the steps are concrete.

The first contacts and assessment
Treatment usually begins with a confidential conversation. The admissions team asks about substance use, mental health symptoms, safety concerns, medications, living situation, and previous treatment. From there, a clinical assessment helps determine whether the person needs detox referral, PHP, IOP, or standard outpatient support.
That first phase should answer practical questions clearly. What level of care fits? How soon can treatment start? Will work or family obligations affect scheduling? What support does the family need right now?
The step-down process
Many people don’t stay at one level the whole time. They start with more structure, then step down as stability improves. Someone may begin in PHP, move into IOP, and later continue with outpatient counseling and recovery check-ins.
This step-down model matters because recovery usually improves in stages. Early on, people often need close support, frequent groups, and more accountability. Later, they need practice maintaining progress with increasing independence.
A few treatment milestones often include:
- Stabilization: Reducing immediate risk, managing cravings, and building attendance.
- Skill development: Learning coping tools, communication skills, and relapse prevention strategies.
- Reintegration: Applying those tools in work, relationships, and community life.
- Aftercare planning: Creating support beyond formal treatment.
Why aftercare matters so much
Finishing a program doesn’t mean recovery is finished. The period after structured treatment can be surprisingly vulnerable, especially if a person loses support too quickly.
According to Outpatient Los Angeles, up to 60% of outpatient completers can relapse within 6 months if they lack a structured alumni network or extended care, and programs with ongoing support can increase one-year sobriety rates by as much as 35%. That’s why aftercare planning shouldn’t be treated as an optional extra.
Strong aftercare may include alumni groups, sober living coordination, family support, recovery refreshers, and regular check-ins after graduation.
The safest discharge plan is rarely “good luck.” It’s a map, a support system, and a next appointment.
Navigating Admissions and Insurance for Rehab
For many families, the hardest part isn’t deciding to get help. It’s figuring out how to pay for it, what insurance covers, and what paperwork comes next. That confusion can slow down treatment at the exact moment speed matters.
What insurance terms actually mean
A few simple terms usually come up during admissions:
- Deductible: The amount a person may need to pay before insurance starts covering certain services.
- Co-pay: A fixed amount owed for a visit or service, depending on the plan.
- Out-of-pocket maximum: The cap on what a person pays during a plan period before covered costs shift more heavily to insurance.
Coverage varies, and every policy has its own rules around levels of care, authorizations, and network details. Some plans cover substantial portions of treatment. Others require more family coordination. People without coverage still have options to explore, and this guide on going to drug rehab without insurance can help frame the questions to ask.
What a smooth admissions process should look like
A strong admissions team should remove friction, not add to it. Families usually need quick answers, plain language, and help gathering the right information.
They should expect support with:
- Benefits verification: Confirming what the insurance plan may cover for treatment.
- Level-of-care guidance: Matching the person to the safest appropriate option.
- Paperwork support: Explaining forms instead of leaving families to decode them alone.
- Start-date coordination: Reducing delays once the clinical need is clear.
The best admissions conversations feel calm and practical. No pressure. No confusing jargon. Just a clear explanation of what’s needed and what happens next.
Choosing a High-Quality Program in Orange County
Once a family decides that outpatient care fits, the next step is choosing carefully. Programs can sound similar from the outside, but the details matter. A high-quality outpatient drug rehab program should offer licensed care, appropriate clinical depth, and a plan that adapts to the individual rather than forcing everyone into the same template.
What to look for
A careful search should focus on a few essentials:
- Licensed and credible care: The program should meet state requirements and operate with clear clinical standards.
- A real continuum: PHP, IOP, outpatient counseling, and coordination for detox or sober living create smoother transitions.
- Dual-diagnosis capability: Substance use and mental health should be treated together when both are present.
- Medication support when needed: MAT access can be essential for some patients.
- Whole-person integration: Mindfulness, movement, nutrition, and experiential care can strengthen long-term recovery.
- Family and aftercare planning: Recovery is more sustainable when support continues beyond the primary program.
Self-motivation also matters. According to Legacy Treatment’s rehab success statistics overview, over 40% of people who successfully complete outpatient rehab decided on their own to seek treatment. That makes compassionate engagement important. Quality programs don’t just wait for motivation to appear fully formed. They help strengthen it through personalized care, clear structure, and respectful communication.
Many families also pay attention to how a center communicates during the first few contacts. Thoughtful intake, responsiveness, and clarity often reflect the quality of care that follows. For readers interested in the broader healthcare side of that issue, these improving patient experience strategies offer a useful lens for evaluating how treatment providers support people in stressful moments.
A strong program should leave a person feeling understood, not processed. In Orange County, that often means looking for care that blends clinical depth with flexibility, practical scheduling, and genuine long-term support.
For anyone considering care for themselves or a loved one, Zoe Behavioral Health offers confidential guidance on outpatient treatment options in Orange County. A simple conversation can help clarify the right level of care, review insurance questions, and outline a recovery plan that fits real life.
