Some evenings follow the same script. He comes home tense, pours a drink quickly, says he’s had a hard day, and promises he’ll keep it under control. By bedtime, the conversation has turned into silence, an argument, or another apology that sounds sincere but changes nothing.
A wife in this position often asks one version of the same question: how to help alcoholic husband without making everything worse. The hard truth is that love alone won’t solve alcohol use disorder. Neither will monitoring, pleading, covering for him, or trying to keep the family calm at any cost.
What helps is a dual-track response. One track focuses on his treatment and accountability. The other protects the spouse’s safety, emotional stability, finances, and future. Those two tracks belong together. When a wife only focuses on saving him, she often disappears inside the crisis. When she focuses only on escape without getting informed, she may miss treatment options that could help.
This guide takes a practical approach. It deals with what to say, what to stop doing, when to seek professional care, and how to support recovery without becoming his manager.
Recognizing the Reality of Alcoholism in Your Marriage
A wife usually knows something is wrong long before she uses the phrase alcohol use disorder. She knows it because dinner plans keep changing around alcohol. She knows it because holidays feel tense. She knows it because she scans his mood when he walks through the door and can tell within seconds whether the night will stay calm.

Heavy drinking versus a disorder
The difference between heavy drinking and a disorder matters. A bad habit can sometimes be changed with willpower and a wake-up call. Alcohol use disorder is a medical condition marked by continued drinking despite harm to health, work, parenting, finances, or the marriage itself.
A husband may still go to work, pay some bills, and insist he’s functioning. That doesn’t rule out a disorder. Many wives get stuck because they’re waiting for a dramatic collapse before they allow themselves to call this what it is.
Common signs that the problem has moved beyond “drinks too much” include:
- Broken promises: He says he’ll cut back, then returns to the same pattern.
- Defensiveness: Simple questions about drinking trigger anger, blame, or shutdown.
- Shifting priorities: Alcohol shapes evenings, weekends, social events, and family plans.
- Repeated fallout: Arguments, missed obligations, risky behavior, or emotional distance keep happening.
- Minimizing: He compares himself to people who are “worse” instead of addressing actual harm.
What helping really means
Many spouses think helping means fixing. It doesn’t. A wife can’t think, argue, or sacrifice her way into making him sober. She can influence the environment around the problem, stop participating in unhealthy patterns, and push the family toward real treatment.
Alcoholism in a marriage is not just his private struggle. It changes the whole home, the emotional climate, and the roles each person starts playing.
That matters because wives often adapt in ways that feel loving but become costly. They smooth things over with children, cancel plans to avoid embarrassment, or stay hyper-alert to prevent a blowup. Over time, the marriage starts revolving around alcohol whether anyone says so out loud or not.
A more accurate starting point
The most useful mindset is this: he may need treatment, and she may need support at the same time. Those aren’t competing priorities. They’re the correct response to a family illness.
When a wife finally names the problem clearly, she can stop asking, “How do I make him act normal?” and start asking better questions. What are the safety risks? What are the consequences of staying passive? What kind of treatment fits his level of need? What support does she need to stay steady while decisions get made?
That shift is painful. It’s also where effective action starts.
How to Talk to Him Without Starting a Fight
Most wives have already tried the obvious approach. They’ve pleaded, warned, reminded, cried, reasoned, bargained, and argued. Research shows 93% of spouses use pleading and 70% use arguing as coping strategies. Those responses make sense. They come from fear, exhaustion, and love. They’re also usually draining, and they rarely produce durable change.

Timing matters more than perfect wording
A serious conversation should never happen when he’s intoxicated, actively withdrawing, rushing out the door, or already escalated. The best window is when he’s sober, relatively calm, and there’s enough time to talk without children hovering nearby.
A wife doesn’t need a flawless speech. She needs a focused one. Long lectures invite denial. Sharp accusations trigger counterattack.
A better opening sounds like this:
“I’m not bringing this up to attack you. I’m bringing it up because your drinking is hurting our home, and I need us to deal with it directly.”
That statement is calm, specific, and hard to sidestep.
What works better than pleading
Structured, supportive communication works better than emotional chasing. The goal isn’t to corner him into admitting everything. The goal is to create a conversation where treatment becomes the next clear step.
Useful phrases include:
- When he minimizes: “Maybe you don’t see it the same way I do, but I do see the impact, and I’m not willing to ignore it.”
- When he says he can handle it himself: “If self-managing were working, we wouldn’t be having this conversation again.”
- When he promises to cut back later: “I’m glad you want things to change. Let’s choose a concrete next step today.”
- When he gets defensive: “This doesn’t need to become a fight. I’m talking about what I will do to protect myself and the family.”
Notice what’s missing. No diagnosing in anger. No stack of old resentments. No threats she won’t carry out.
Keep the conversation tied to action
One of the most effective moves is to ask for one immediate commitment instead of demanding a total personality transformation overnight.
Examples:
- Ask for an assessment: “Will you speak with a treatment professional this week?”
- Ask for one sober block of time: “Will you agree not to drink before family dinner for the next few days?”
- Ask for practical cooperation: “Will you let me help arrange an evaluation so we know what level of care makes sense?”
What to avoid in the moment
Some responses feel natural but backfire fast.
| Less effective approach | Better alternative |
|---|---|
| “You always ruin everything.” | “Your drinking affected the kids and the evening, and that can’t keep happening.” |
| “If you loved us, you’d stop.” | “Love isn’t the issue. The issue is that this needs treatment and accountability.” |
| “This is your last chance,” when she isn’t ready to follow through | “Here is the boundary I’m setting, and here’s what happens if it’s ignored.” |
A wife doesn’t need to be cold. She does need to be clear. Calm language lowers heat. Clear language raises accountability. That combination gives the conversation its best chance.
Setting Boundaries and Stopping the Cycle of Enabling
When a wife asks how to help alcoholic husband, she often means, “What can she do that helps instead of inadvertently feeding the problem?” That question usually leads to one uncomfortable topic: enabling.
Enabling isn’t love. It’s any pattern that shields him from the impact of his drinking. That might mean calling his boss with an excuse, handing over money, cleaning up a mess he created, or pretending the children didn’t notice what they absolutely noticed.
Boundaries are protection, not punishment
A boundary is not a speech about what he should do. It’s a statement about what she will do in response to behavior that harms her or the family. Anyone who needs help with understanding boundaries in relationships can benefit from reviewing what healthy limits look like in practice.
A boundary sounds like this:
Practical rule: “If you’ve been drinking, you won’t drive the children, and if you try, I will take the keys and arrange other transportation.”
That is concrete. It is enforceable. It protects people.
Compare that with a vague line such as, “You need to start being more responsible.” True, but useless. It doesn’t define any action.
Stop doing this and start doing this instead
Many spouses know something has to change, but they need a side-by-side replacement for the habits they’ve fallen into.
- Stop covering for him. Start telling the truth in simple terms. If he misses an event because he was drinking, don’t invent another story.
- Stop rescuing him from every consequence. Start allowing natural outcomes to land when safety permits.
- Stop giving cash that can disappear into alcohol. Start paying only for essential needs directly, if needed at all.
- Stop debating whether it was “that bad.” Start responding to the behavior that happened.
- Stop making the whole house revolve around his mood. Start organizing life around stability for children and for the spouse.
A useful companion resource on this distinction is enabling vs helping and what the difference looks like in addiction.
Boundaries require follow-through
The hardest part isn’t setting a boundary. It’s keeping it when he gets angry, tearful, charming, or full of promises. A boundary without follow-through becomes another scene in the cycle.
For example, if she says, “I won’t stay in the room when you’re drunk and hostile,” then she needs an exit plan. That may mean sleeping elsewhere in the house, going to a relative’s home, or calling for support. If she says, “I won’t loan money for alcohol-related emergencies,” then she can’t reverse course because he sounds desperate.
Healthy boundaries often produce more conflict at first, not less. That doesn’t mean they’re wrong. It usually means the old system is being disrupted.
Safety comes first
Not every marriage is safe enough for direct boundary-setting without support. If he becomes threatening, physically intimidating, reckless, or violent, the spouse’s priority is immediate safety, not the quality of her phrasing.
A wife doesn’t need permission to protect herself. She also doesn’t need to wait until she feels emotionally ready. Boundaries are one of the most loving actions available because they stop the marriage from organizing itself around denial.
Finding Professional Treatment That Actually Works
At some point, a serious alcohol problem needs more than insight and better conversations. It needs treatment. That’s where many families get stuck. They know he needs help, but the treatment system feels confusing. They hear words like detox, outpatient, therapy, medication, family sessions, and relapse prevention, but they don’t know what fits his situation.
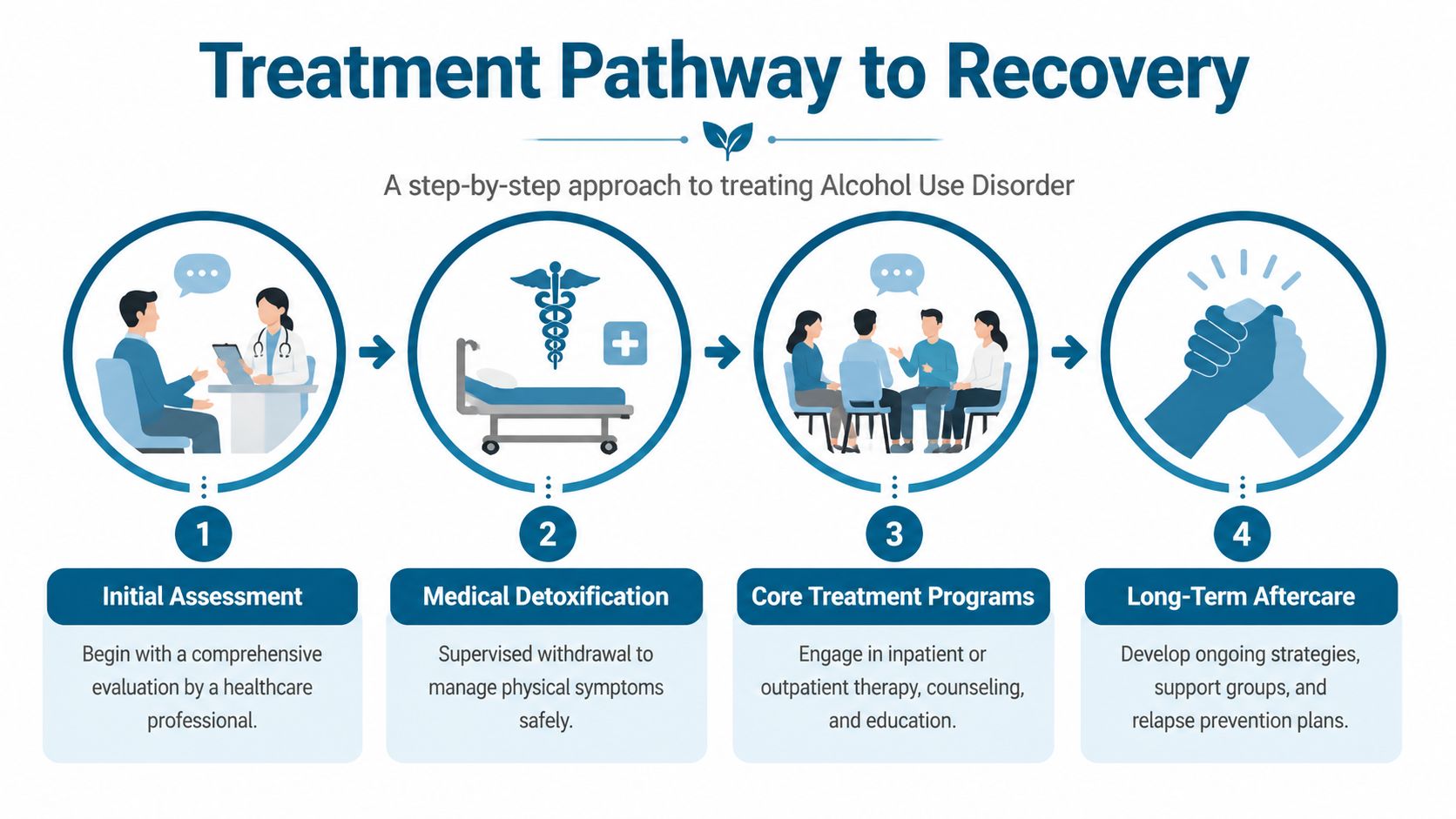
Start with the right level of care
The first question is not, “What program sounds nice?” It’s, “What level of care is medically and clinically appropriate?”
A practical pathway often looks like this:
Clinical assessment
A professional evaluates drinking patterns, withdrawal risk, mental health symptoms, home stability, and prior treatment history.Detox referral when needed
If he’s physically dependent on alcohol, withdrawal can be dangerous. In that case, medical detox comes first.Structured treatment program
After stabilization, he may need daily or near-daily treatment rather than occasional counseling.Aftercare and recovery support
Long-term change requires a plan after the initial program ends.
For families comparing programs, this guide on choosing a rehabilitation facility with the right questions can help narrow the decision.
Why outpatient care often fits family life
Not every husband needs to live away from home for extended treatment. Many do best in a structured outpatient model after detox or as a direct entry point when medically appropriate. That’s especially important for families trying to balance parenting, work, and treatment access.
Two levels often matter most:
| Level of care | What it usually looks like | When it can help |
|---|---|---|
| PHP | Treatment for much of the day, several days a week, with strong clinical structure | When he needs intensive support but not round-the-clock residential care |
| IOP | Fewer weekly treatment hours than PHP, with continued therapy and accountability | When he’s stable enough for more independence but still needs substantial structure |
For many Orange County families, outpatient treatment reduces logistical barriers. A husband can receive intensive care during the day and sleep at home at night, while still rebuilding routines in real life rather than in isolation from it.
Dual-diagnosis care matters
A major reason treatment fails is that alcohol isn’t the only problem. Depression, anxiety, trauma, and other mental health concerns often drive drinking and complicate recovery. According to guidance on dealing with an alcoholic spouse, over 50% of people with alcohol use disorder also have a co-occurring mental health condition, and dual-diagnosis care has been associated in California with 25% higher program retention compared to addiction-only care.
That changes the treatment conversation. If a husband drinks to numb panic, trauma symptoms, or persistent depression, then asking him to “just stop” without addressing the psychiatric piece is incomplete care.
Effective treatment should assess questions like these:
- What is alcohol doing for him emotionally?
- What symptoms show up when he’s sober?
- Does he need psychiatric evaluation or medication support?
- Has unresolved trauma become part of the relapse cycle?
Family involvement improves outcomes
A spouse should also look for treatment that involves the family, not just the identified patient. According to outcome data on alcohol rehab and family therapies, evidence-based family therapies such as Alcohol Behavioral Couples Therapy can double the chances of maintaining abstinence compared with individual counseling alone.
The best treatment plans don’t treat alcohol in a vacuum. They address the marriage, the home environment, communication patterns, relapse risk, and co-occurring mental health needs.
That doesn’t mean a wife becomes his therapist. It means quality care gives the couple structured help around trust, conflict, routines, and support.
What a spouse should ask a treatment program
Before enrolling, a wife should ask direct questions:
- Assessment: How do clinicians determine whether detox, PHP, or IOP is appropriate?
- Mental health: How is dual-diagnosis care handled if depression, trauma, or anxiety are present?
- Family therapy: Are spouses included in treatment planning and counseling?
- Medication options: Is medication-assisted treatment discussed when clinically appropriate?
- Transition planning: What happens after the initial phase of treatment ends?
A treatment center that can answer those questions clearly is operating from a serious clinical framework, not wishful thinking.
Supporting His Recovery and Rebuilding Your Relationship
Getting him into treatment is not the finish line. Early recovery can be awkward, hopeful, frustrating, and fragile all at once. A wife may feel relief that he’s finally getting help, then feel angry that trust doesn’t magically return. Both reactions are normal.

Healthy support is different from management
Recovery works better when the spouse is supportive without becoming the recovery police. He needs accountability, but he also needs to own his program.
Support often looks like:
- Making room for treatment commitments such as therapy, groups, or recovery meetings
- Creating a lower-risk home environment by reducing alcohol-centered routines
- Encouraging honesty about stress, cravings, and setbacks
- Participating in family sessions when invited by clinicians
Management looks different. It includes checking his phone, interrogating him nightly, tracking every minute, or trying to personally enforce sobriety. That role burns out the spouse and weakens his responsibility.
Trust rebuilds through patterns
Apologies matter, but patterns matter more. A wife doesn’t have to “move on” because he’s newly sober. Trust returns when behavior changes consistently over time. He tells the truth. He keeps commitments. He participates in treatment. He responds to stress differently. He accepts limits instead of fighting them.
A couple often needs help learning how to relate without alcohol at the center. That’s one reason family-involved treatment is so important. As noted earlier, evidence-based couples work is linked with stronger abstinence outcomes than individual counseling alone. The clinical reason is simple. The marriage itself becomes part of recovery rather than a backdrop to it.
Prepare for strain without predicting failure
Not every hard week means relapse. Not every relapse means treatment failed. Recovery usually requires a different mindset from both partners.
“Support sobriety. Don’t carry it for him.”
A practical home plan can help. Keep it simple and specific:
- Discuss triggers openly: social events, work stress, isolation, and conflict should be named early.
- Agree on a response plan: if cravings rise or warning signs return, know who he contacts and what he does next.
- Protect routines: regular sleep, meals, movement, and treatment attendance make a difference.
- Keep children out of adult recovery roles: they shouldn’t monitor, report, or calm a parent’s addiction.
Rebuilding the marriage takes separate healing too
Some wives discover that once the chaos settles, grief finally catches up. They may feel anger about years lost, lies told, or fear absorbed by the family. That doesn’t make them unsupportive. It means the marriage has injuries that sobriety alone won’t erase.
Recovery can absolutely improve a relationship. But a stronger marriage usually comes from two things happening together. He works on sobriety and emotional accountability. She works on safety, clarity, and her own healing. Then the relationship gets rebuilt on current behavior, not on promises made in crisis.
Prioritizing Your Own Well-being and Finding Support
Many wives delay caring for themselves because his drinking feels more urgent. They tell themselves they’ll rest after he gets sober, make a therapy appointment after the next crisis passes, or ask for help once the house calms down. That logic is common, and it keeps them trapped.
A spouse living with alcoholism often becomes the emergency system for the family. She monitors tone, schedules, finances, excuses, and fallout. Then she wonders why she feels anxious, numb, angry, ashamed, or exhausted. The answer is simple. She has been living in a chronic stress environment.
Your well-being is not a side issue
Spouses of alcoholics are often described as overlooked victims. According to clinical guidance on the effects of living with an alcoholic spouse, they face a higher risk of domestic violence, health problems, and emotional trauma, and support groups like Al-Anon are designed specifically to provide peer support and coping strategies for family members.
That means self-care is not cosmetic. It is protective. It is part of crisis response.
Signs a wife needs immediate support include:
- Constant hypervigilance: She’s always scanning for danger or the next disruption.
- Isolation: She has stopped telling the truth to friends or family because she feels embarrassed or defeated.
- Physical strain: Sleep problems, headaches, stomach issues, or panic symptoms are becoming common.
- Fear at home: She changes her behavior to avoid setting him off.
- Loss of self: Her days revolve around managing his condition instead of living her own life.
Build a support structure that doesn’t depend on him
Support has to come from outside the marriage too. A strong plan often includes individual therapy, trusted family or friends, and a peer group such as Al-Anon.
For broader emotional education, some spouses also benefit from a free anxiety education hub that helps them understand how chronic stress can affect the body and mind. That kind of resource isn’t treatment by itself, but it can help a person recognize that what she’s feeling has a name.
A family-specific recovery resource such as support for families of addicts can also help spouses think through practical and emotional next steps.
Practical protection matters too
Emotional support is not enough if the situation is unstable. A wife may also need to review basics that are easy to avoid when overwhelmed.
Consider these areas:
- Financial clarity: Know what accounts exist, what bills are due, and whether money is disappearing.
- Child safety planning: Decide who can help with transportation, school pickup, or emergency care if he’s impaired.
- Legal awareness: If there has been violence, threats, reckless driving, or repeated instability, legal advice may be necessary.
- Exit planning: Even if she hopes to stay, she should know where she could go and who she could call if the home becomes unsafe.
The most important shift
A wife cannot control whether her husband accepts recovery. She can control whether she keeps living without support, without boundaries, and without a plan. That shift often changes everything.
When a spouse gets stronger, the whole system changes. She speaks more clearly. She reacts less impulsively. She follows through. She stops organizing reality around his denial. Ironically, that often creates the conditions where treatment becomes more likely because the family is no longer absorbing the full cost of his drinking.
Hope is still possible. But hope works best when it’s attached to action, protection, and professional care rather than wishful waiting.
When a husband needs real help for alcohol use and the family needs a path forward, Zoe Behavioral Health offers a strong outpatient option in Orange County. Their team provides confidential admissions support, insurance verification, referrals for detox when needed, and personalized treatment planning that can include PHP, IOP, dual-diagnosis care, family support, and ongoing recovery guidance. For spouses trying to figure out what to do next, reaching out for a private consultation can turn confusion into a concrete plan.
